ENTER YOUR EMAIL TO RECEIVE OUR WEEKLY NEWSLETTER
Healing Power of Music
Music therapy offers balm to the sick and may spark recovery for patients with severe impairment.
By Deborah Harkins
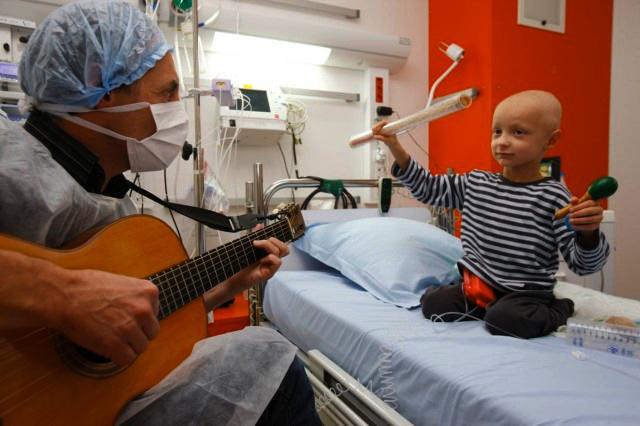
Music therapy in children’s cancer ward in France. Photo by Pascal Deloche/Godong/Corbis
. . . . . . . . . . . .
It was now or never. The patient, a 76-year-old laundress in the Dominican Republic, was scheduled for total bilateral knee replacements. But her blood pressure was so high—240/120—that her surgical team refused to operate. The patient’s face was contorted with worry. She couldn’t simply put off the procedure: The operation was part of a philanthropic program; her surgeons would not return to her hospital in Santo Domingo for a year at the earliest. And aggressive drug therapy was not bringing the pressure down.
The solution, it turned out, was song. In her room, the patient, a deeply religious woman, asked her nurses tentatively, “May I sing?” (She was worried about disturbing her three roommates.) After she’d crooned only two religious songs, her blood pressure dropped to 180/90. With her nurses’ hearty endorsement, she sang softly through the night; the next morning she was cleared for surgery. She had successful total knee replacements, wrote the doctors who published her case history in Arthritis Care & Research (April 2011).
Why does old-fashioned music sometimes succeed when state-of-the-art medicine is at a loss? “In a very specific way, music can excite areas of the brain that have been dormant; it can turn on verbal or visual pathways that cannot be accessed by other therapies,” notes Dr. Concetta Tomaino, D.A., MT-BC, LCAT , a pioneer in the deployment of music to spark recovery in patients with severe disabilities. Dr. Tomaino is the co-founder, with the late neurologist Oliver Sacks, of the Institute for Music and Neurologic Function (IMNF) at Beth Abraham Family of Health Services in the Bronx. Its mission: to study “music’s extraordinary power to awaken, stimulate and heal.”
We’ve all seen music work its magic in our everyday lives. Recently I followed two professional guitarists and a soprano around a patient floor at Roosevelt Hospital—and saw singing bring patients instant ease and trigger deep emotion. These musicians were among the many professional players who volunteer to bring live performances to patients and caregivers in six New York City health-care facilities through Sing For Hope. “Do you care for a song?” the trio would ask, pausing in the patient’s doorway; about half the time, they’d be invited in.
Our most enthusiastic welcome came from a jovial elderly woman who wanted to hear “A Bushel and a Peck.” After the team launched into it, soprano Catherine Hancock began singing “Someone to Watch Over Me.” As the soothing melody pervaded the room, the patient relaxed and lay back, transported; her eyes closed as she silently mouthed the words. When the song was over, she told us, in a choked voice, that its message had affected her deeply; it had brought back memories of how she had watched over her husband in his illness, and it made her hope that the next day, during her operation, “God will be watching over me.”
What the Sing for Hope musicians were offering patients that day was “therapeutic music”—music that any laymen can provide to give moments of respite to those who are sick. But “music therapy,” Dr. Tomaino points out, is a tool employed in a serious effort at rehabilitation, and those who practice it have undergone rigorous academic training. “Most people don’t think of music therapy as a health-care field,” Dr. Tomaino says. “But it is.”
During the 16 years she has worked at the Institute for Music and Neurologic Function with patients suffering from stroke, traumatic brain injury, and chronic diseases like Parkinson’s and multiple sclerosis, Dr. Tomaino has seen music stimulate the memory of patients suffering from dementia; help stroke patients recover their power of speech; aid physical therapists strengthen the muscles of patients and extend their flexibility; assist Parkinson’s patients regain their ability to walk; and reduce severe anxiety in pre- and post-surgery patients. In a series of short, compelling videos, Dr. Sacks speaks eloquently of the transformations that he and Dr. Tomaino have witnessed over the years (see “Music Has Charms…” below).

Dr. Concetta Tomaino sings with dementia patients earlier in her career
at Beth Abraham. Photo by Roberta Hershenson.
. . . . . . . . . . . .
The New Science of Song
All of us can use music to bring pleasure to the sick; music therapists, however, know how to use music to treat patients. With guitar, keyboard, drums, or accordion (Dr. Tomaino’s instrument of choice), these specialists work in hospitals, nursing homes, rehab centers, schools, and hospices—and their expertise is available to patients at home as well. (See “Harnessing Music’s Restorative Power”, next page.) They work with special-needs children, people suffering from depression or dementia, patients disabled by accident or brain injury, and the dying. And they have credentials: A music therapist must be a proficient musician and college graduate with a degree in music therapy; he or she must have spent at least 1,200 hours in clinical training, including a supervised internship; passed a national certifying examination, and, in New York State, be licensed.
“An ordinary musician can sing along with a patient with aphasia, but he won’t know why she can sing, say, only the first and last words of “By the Light of the Silvery Moon,” explains Dr. Tomaino. “A music therapist [MT] will alter the music, perhaps exaggerating the range of the note where a patient gets stuck, and then have the patient repeat the phrase over and over until the repetition disinhibits the block in her brain. Then the MT will prepare a treatment program and monitor the patient’s progress.
“Parkinson’s patients have trouble initiating steps, cadence, and balance,” she continues. “People assume that if they play rhythmic music, a patient will follow it. But Parkinson’s patients don’t perceive the beat the way others do. MTs are trained to manipulate the beat until they see that the patient can feel it. And to help Parkinson’s patients with their speech, MTs will initiate vocalization: Since a patients’ vocal folds atrophy, one way to keep them soft is humming.”
Dr. Tomaino’s institute has CDs of “amazing” music that patients have created—therapists at IMNF urge patients to compose music and lyrics to help them deal with post-injury depression. “Music can be used in an in-depth, therapeutic way,” Dr. Tomaino notes. “It helps the body break through some of the inhibitions that result from traumatic injury. Many times patients can’t articulate what they are going through. Composing helps them do that.” She cites a young man who had lost both of his arms as a result of gang violence. After months and months of therapy, he composed a song that declared, “Life isn’t what you expect, but it’s a brand-new day.”
Today, advances in brain imaging enable researchers to chart the pathways that music follows in the brain. In her new book on the power of music, Elena Mannes, granddaughter of the founders of New York City’s Mannes College of Music, calls this research “the new science of song” (see “Breakthrough Moments in Music Research” below).
And research—the randomized, controlled trials that are the gold standard of scientific study—has begun to validate what we laymen “know” and what clinicians like Dr. Tomaino have long observed: Music therapy can improve the medical outcome of patients with many different afflictions. The field is young: Many of these trials involve only small numbers of patients, and authors of the studies stress the need for further research. Still, using rigorous research methods, these small trials have shown that music therapy can, among its other benefits, lower blood pressure preoperatively and relieve depression. It may help children with autistic spectrum disorder improve their communicative skills, and help people with schizophrenia improve their global state. On music therapy’s effectiveness in pain relief, a 2006 review of 51 studies concluded, “Listening to music reduces pain intensity levels and [morphine and other opioids], but the magnitude of these benefits is small and, therefore, its clinical importance unclear.”
Music and Dementia
“Most people are just awed by the power of music to awaken a person with Alzheimer’s disease,” says music therapist Al Bumanis, a spokesman for the American Music Therapy Association in Silver Spring, Maryland. Many dementia patients who can no longer speak or recognize faces show a heartening—and startling—response to “their kind of music.” They sing along with the melody. Or, if they don’t sing, they mouth the words. “The reawakening of the connection between patient and caregiver when they’re singing together can be very moving,” Bumanis says.
“It is well established that music is a very important tool in reaching people with dementia—even in the advanced stage,” points out Jed Levine, director of programs for the New York City chapter of the Alzheimer’s Association. “There is evidence that the ability to hear and the ‘center for music’ remain active. At all stages of the disease, music can provide stimulation as well as solace and comfort.”
To break through to someone locked in dementia, Levine points out, a friend or caregiver must choose melodies that have particular significance for that person. The music that resonates most strongly for most of us, notes Dr. Tomaino, is the music we heard as teenagers—although “classical-music fanatics” respond most fervently to a particular opera or the work of a particular composer.
A 2001 study at McGill University clarified just how exquisitely particular musical taste can be. Ten classical musicians claimed that their favorite piece of music sent chills down their spine. This is quite likely, since music—like sex, cocaine, and other abused drugs, and food—triggers the area of the brain that releases dopamine, a neurotransmitter associated with feelings of pleasure and reward. The McGill researchers were intrigued: Would musicians get spine-shivers from other people’s favorite classical pieces? Would these “control” pieces trigger the pleasurable responses signified by changes in cerebral blood flow with the same intensity of emotion and arousal? Would they, too, spark what neuroscientist Daniel Levitin calls “goosebumps on the brain”
The answer was “no.” The participants found spine-tingling pleasure only in their favorite pieces. The moral: If musical taste is this selective, then it’s clear that a melody will stir or comfort or stimulate a patient with dementia—indeed, any patient—BUT only if it’s his kind of music.
Harnessing Music’s Restorative Power
There are many ways to bring the pleasures of music to hospitalized or homebound friends or family members—whether or not you’re the sort who’s comfortable launching into a song at bedside.
Bring in a playlist of songs customized by a specialist to strike the strongest emotional chord. The Institute for Music and Neurologic Function’s Well Tuned: Music Players for Health program (a collaboration with another nonprofit, Music & Memory) can help you discover which songs will resonate with a patient. A licensed musical therapist will consult you by phone about the patient’s musical taste, then load an MP3 or iPod with a customized playlist of therapeutic music. (Playlists can be created for individuals with Alzheimer’s disease and other forms of dementia; Parkinson’s disease; depression; or anxiety.) For details and fees, visit their website. To donate your working iPod or MP3 player (with cable or dock) for this purpose, call the institute at 914-513-5292.
Many sick or elderly patients are too agitated to put on headphones or keep earbuds in their ears. The Well Tuned program’s specialist can suggest alternative speaker options or iPod docks; indeed, there’s even a “pillow speaker” (a pillowcase safely wired with headphones), which the patient can use if the hospital staff gives permission.
Use music to reach the dying. Asked about music’s ability to provide comfort at the end of life, Tomaino says fervently, “It’s a boon to all the family members. It helps with pain and stress, helps the patient feel at peace. And if she’s alert, it can help her with life transition issues—help her say to her loved ones what she wants to say.
“Family members often say to me, ‘I go into the room, and don’t know what to say. It’s so stressful and awkward; I take the kids, and what do we do?” I tell them, ‘Take the kids and help them choose music that will help them express what they want to express.” A music therapist can help with this—help family members pick the music that says what they want to say. Even if the patient is minimally responsive, he will experience, through music, that family members are conveying emotion to him.
Sing to the patient, Dr. Tomaino urges. “Many say they can’t sing, but if they do it as a group, there’s usually no problem. And when they do choose a song, it’s usually something that’s very poignant. More times than not, the family members are very grateful for being able to have that experience.”
Call in a music therapist. When the patient’s suffering is acute—when he or she urgently needs a respite from pain, agitation, depression, isolation—consider calling on a licensed music therapist to kindle the release from anxiety and the surge of endorphins that music bestows. There may be such a professional on the hospital’s staff; if not, you can locate one through the American Music Therapy Association (AMTA). In New York City the hourly fee ranges from about $60 to about $95. Some music-therapy treatments are reimbursable through Medicare, Medicaid, or private insurance; see the FAQ page on the AMTA’s website for details.
Recently, the Institute for Music and Neurologic Function inaugurated a program offering private sessions in the patient’s home or medical facility through its Music Therapy Professionals Practice. The IMNF’s music therapists work with patients in many different areas: memory enhancement, movement and speech rehabilitation after traumatic brain injury, pain management, early-childhood intervention, medical psychotherapy (aid in dealing with the stresses involved with serious illness)—and they’ll also train caregivers in how to use therapeutic music to help their loved ones. In New York City the hourly fee ranges from about $60 to $100 for a 45-minute session (price not updated for 2018…ed).
For caregivers, too, music has restorative power. Singing in a chorus, after all, triggers the brain to release the “pleasure and reward” chemical, dopamine. So does a night at the Philharmonic, at a jazz club, in an Irish pub…wherever you’ll find the sort of music—sublime, sacred, plaintive, effervescent—that resonates with you.
. . . . . . . . . . . .
MUSIC HAS CHARMS…
…to soothe the agitated, un-freeze the transfixed, restore memory to those who’ve lost their past, give language to the speechless. Eloquently, exuberantly, neurologist Oliver Sacks explains that healing power in a series of brief YouTube videos that capture the wonder at the power of music that comes through so clearly in his book Musicophilia: Tales of Music and the Brain. Perhaps his most compelling video is the one in which he describes how music can relieve the torment of patients suffering from aphasia after stroke. The therapy may take 70 to 80 hours of intensive effort, he says, “but to regain language, one would give one’s soul.”
BREAKTHROUGH MOMENTS IN MUSIC RESEARCH
Noted neurologist Oliver Sacks, professor of neurology and psychiatry at Columbia University Medical Center, lays out fascinating case histories that explore the human brain’s susceptibility to music in Musicophilia: Tales of Music and the Brain. Daniel Levitin, director of the Laboratory for Musical Perception, Cognition, and Expertise at McGill University, in Canada, provides a detailed but understandable primer on how the brain processes music in his well-reviewed 2006 book This Is Your Brain on Music. And Elena Mannes, whose grandparents founded the Mannes College of Music, discusses breakthrough moments in music research (“the new science of song”) in her new book The Power of Music.
. . . . . . . . . . . .
Deborah Harkins, an editor at Women’s Voices for Change, was an assigning editor at New York magazine for more than 20 years, the articles editor of The Modern Estate, a columnist for The New York Daily News, and associate editor at NYCitywoman.com.